You don’t need to have a formal trauma diagnosis to know that something’s off. Maybe you’re constantly overwhelmed even when nothing dramatic is happening. Or you find yourself shutting down in situations that don’t seem “bad enough” to explain the intensity of your reaction. You sleep, but never feel rested. You “hold it” together all day and feels at peace only when you’re alone.
This kind of stuckness is more than ordinary stress. And it’s something I see often in my work as a trauma therapist, particularly with women who’ve spent years managing symptoms without ever being given a name for what they are feeling.
One helpful way to understand these trauma patterns is through the lens of threat stress and challenge stress. These aren’t labels or diagnoses, just two different ways our nervous system can experience stress. And the difference between them matters, especially for those living with the long-term effects of complex trauma or CPTSD (even if they’ve never used those terms).
Two Kinds of Stress
Our bodies are wired to respond to stress. That’s a good thing. It helps us survive. But the way we experience stress can shape how we feel, how we function, and how safe we feel in our own skin.
Challenge stress happens when something is hard, but manageable. You feel stressed, but there’s a sense you can get through it. Your body gets activated. Heart rate goes up, attention is sharpened, but then it settles. You feel tired after, but not lost. There’s a sense of movement, of direction. Threat stress is different. It’s what happens when you sense danger, even if nothing looks obviously threatening on the outside. It’s the kind of stress that feels inescapable, unpredictable, or never-ending. You freeze, go blank, or feel your heart race without knowing why. Or you manage to power through the day, only to collapse later.
For people with trauma histories, especially complex trauma from childhood or relational harm, this kind of trauma response can become the norm. Your nervous system doesn’t wait to check if you’re safe. It responds as if the worst is already happening.
Signs of Living in Survival Mode
When this state of trauma-related stress has been part of your life for a long time, it can feel ordinary. You notice a low level of tension that rarely fades. Or moments of numbness when everything flattens and you go through the motions. And things that seem small to others might feel like too much; not because you’re weak, but because your body is already doing so much just to hold steady.
You may find yourself constantly thinking ahead, scanning for what could go wrong, or needing to stay busy to avoid stillness. Or you look calm on the outside, yet inside, there’s a tightness you can’t quite explain. It’s not all in your head, it’s in your body too.
These aren’t personal failures. These are patterns that began as protection, ones your trauma-affected system hasn’t yet learned how to let go of.
Where These Patterns Come From
For many people, these trauma responses don’t appear out of nowhere, they are built over time. Often, they start in childhood, during moments or years when a child doesn’t feel consistently safe or seen. The brain and body adapt in smart, protective ways: staying alert, learning not to expect support, bracing for what might come next.
Even when adult life seems different on the outside, the nervous system can remain tuned to threat. It’s like the dial was set years ago and hasn’t been adjusted. You feel like you are overreacting, but it is your system doing what it learned to keep you safe in a world that didn’t always feel safe.
Over time, these trauma-related patterns can become automatic. And the more often they’re activated, the more familiar, even necessary, they can feel. This is what makes healing such slow work: it’s not about pushing through, but slowly showing your body and mind that it can begin to let go.
What This Can Look Like Day-to-Day
Imagine this: you’re at a social event where you don’t know many people. You see someone you’d like to talk to, maybe they seem kind or approachable. Part of you wants to walk over and say hello. But your body freezes. Your heart races. You suddenly feel awkward and exposed. Before you’ve taken a step, your mind floods with reasons not to: What if I bother them? What if they look at me strangely? What if I say something stupid?
So you stay put. You scroll through your phone or head to the loo. You tell yourself it’s not a big deal. Maybe it isn’t, logically. But it doesn’t feel small. It feels like danger. Not because anything bad is actually happening, but because you are reacting to a much older, much deeper fear: that reaching out isn’t safe. That you’ll be rejected, judged, or hurt again.
This kind of moment might seem minor on the surface, but it speaks volumes about how the nervous system has learned to protect you. It’s not about social confidence. It’s survival shaped by past trauma. And that reaction, quick, intense, and hard to override, isn’t your fault.
This isn’t about meeting new people. It’s about your nervous system interpreting a neutral moment as something more. Perhaps it reminds your body, without words, of a time when being visible or getting something wrong had consequences. That old threat doesn’t need to be named for it to resurface. And you respond just as you did back then: protectively, urgently.
Moments like this can be baffling and can feel like personal failure. But they’re not. They’re signs that your body remembers what it learned and hasn’t yet had a reason to unlearn it.
Returning to Challenge Stress
Understanding the difference between threat and challenge stress doesn’t solve everything, but it does offer a new way to see your trauma-related experience. It can help explain why some situations feel unmanageable even when they seem small, or why your reactions catch you off guard.
In trauma therapy, we often begin by getting curious about these responses; not trying to change them straight away, but noticing them. Over time, this helps build the foundation for something new. You start to notice moments when the stress doesn’t immediately feel like danger. You might notice the fear is there, but you are able to stay present. A small sign that your body is beginning to respond differently. That’s the possibility of challenge stress. The goal isn’t to eliminate stress altogether. That’s not realistic. What matters more is helping your body and mind recover more easily and respond with greater flexibility.
For many people with complex trauma, this move from threat to challenge marks a quiet but meaningful change. It doesn’t always come with fanfare, but you feel it: a little more steadiness, a little more room to breathe.
Before going further, it helps to look briefly at what’s happening in the brain during these moments of overwhelm.
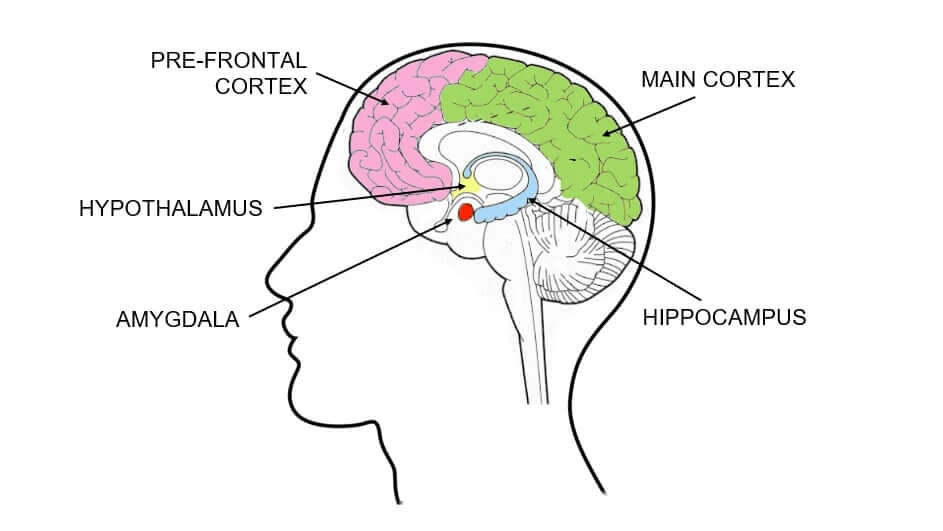
The amygdala, deep in the brain, plays a key role. It’s like a smoke alarm, quick to signal when something feels off. When it fires, your body prepares to act: heart rate rises, muscles tense, and your focus narrows. But this reaction doesn’t always match the reality of the moment. That’s because the prefrontal cortex, which is the part of the brain responsible for assessing context and making decisions, gets quiet when the amygdala takes over. You might know there’s no real danger, but your system doesn’t feel that way. Then there’s the hippocampus, which helps differentiate past from present. When it’s been affected by trauma, it may struggle to remind you that what’s happening now isn’t the same as what happened then. As a result, your body responds as though an old threat is happening again. Right here, right now.
None of this means you’re broken. It means you are doing exactly what you were trained to do. Sometimes too well. We are not trying to achieve a life without stress, but we are helping your system find its way back to balance more easily after it’s been activated.
Reframing
What if your overwhelm isn’t a weakness, but a message from a nervous system that’s been doing its best to protect you? What if the first step isn’t about fixing anything, but about noticing and naming what’s happening inside? This isn’t about becoming someone new. It’s about slowly returning to parts of yourself that got tucked away while you were just trying to stay safe.
Further Reading
Neuroscience and Clinical Research
- McEwen, B. S. (2007) – Physiology and neurobiology of stress and adaptation: Central role of the brain
Physiological Reviews, 87(3), 873–904.
A foundational paper on how chronic stress reshapes brain structure and function — including the hippocampus, amygdala, and prefrontal cortex. - Teicher, M. H., & Samson, J. A. (2016) – Enduring neurobiological effects of childhood abuse and neglect
Journal of Child Psychology and Psychiatry, 57(3), 241–266.
Explains how early relational trauma disrupts emotional and cognitive development, often leading to long-term changes in the stress response. - Harvard University – Center on the Developing Child
developingchild.harvard.edu
Clear, research-informed resources on how childhood adversity affects brain development and regulation.
Accessible, Trauma-Informed Books
- Bessel van der Kolk – The Body Keeps the Score
A widely respected book on how trauma affects both the mind and body — and how integrative approaches can support recovery. - Deb Dana – Anchored: How to Befriend Your Nervous System Using Polyvagal Theory
A compassionate and practical introduction to recognising and regulating your own nervous system responses. - Peter Levine – Waking the Tiger: Healing Trauma
Describes how trauma becomes held in the body and how it can be released through gentle, somatic attention. - Pat Ogden – Sensorimotor Psychotherapy: Interventions for Trauma and Attachment
A therapist-focused yet readable guide that explores how trauma shows up in posture, movement, and sensation — especially in relational contexts. - Stephen Porges – The Pocket Guide to the Polyvagal Theory
Explains the role of the vagus nerve and how connection, safety, and social cues shape our physiological state.







